
April • 30 • 2021
Insights From 10 Years of Malpractice Claims Data: Part IV
Summary
Coverys’ special report, A Call for Action: Insights From a Decade of Malpractice Claims, examines data derived from 11,000+ events pertaining to 20,000+ closed claims across a 10-year period (2010 to 2019). This is the fourth of a five-part blog series based upon the report.
There is wide awareness of tenacious threats to healthcare and the tools and tactics in place to prevent them. Awareness, however, has not always translated into action. Fortunately, there is growing openness toward sharing stories, collecting data, and distributing knowledge to help address these threats. There is also continued interest from organizations and clinicians to examine their own claims data and adverse events to help reduce risk and improve patient care.
This article highlights claims data related to key existing risks that exhibit flat trends or in some instances are slightly increasing. These include: communication, retained foreign bodies, and hospital-acquired infections.
Communication
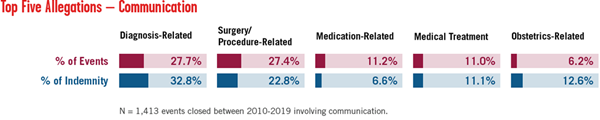
The top three allegation categories for communication risk are diagnosis-related, surgery/procedure-related, and medication-related. Within diagnosis-related events, the most common are history/physical and assessment of the patient, test interpretation, and ordering diagnostic/lab tests for cancer, cardiac/vascular, and infection conditions. Performance is the most frequent and costly communication issue in surgery allegations, especially for orthopedic and general surgery. Monitoring/management, ordering, and administration of medication are issues in medication-related allegations.
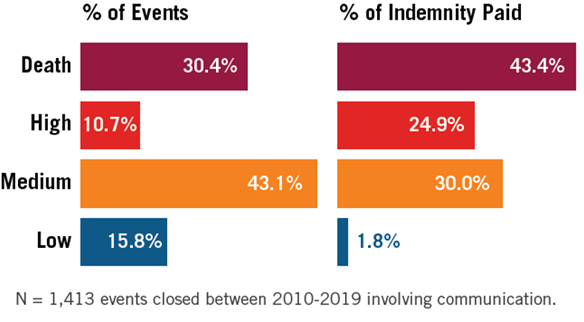
Slightly more than 41% of events related to communication issues resulted in death or high-injury severity.
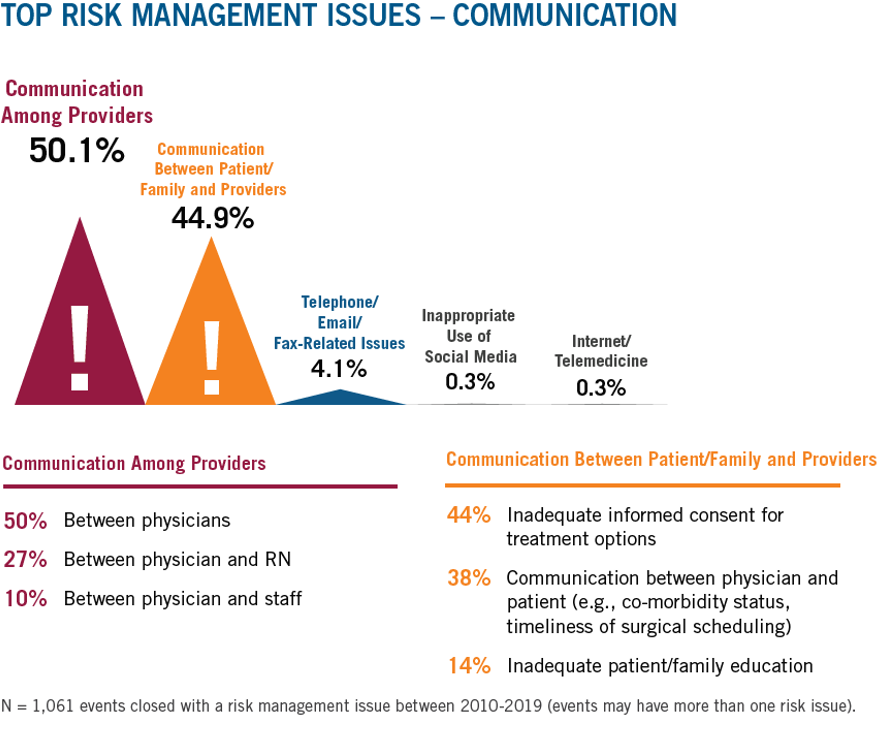
Retained Foreign Bodies
Retained foreign bodies include sponges, needles, and equipment. The overall volume of retained foreign body events is low (228 events from 2010-2019), but average paid indemnity is increasing. Technology has been developed to help reduce this risk, but even this number of claims and suits begs the question of widespread adoption. Rigid adherence to counting, the use of X-rays, bar code technology, and small teams of surgical staff focused on preventing retained foreign bodies can help reduce this risk.
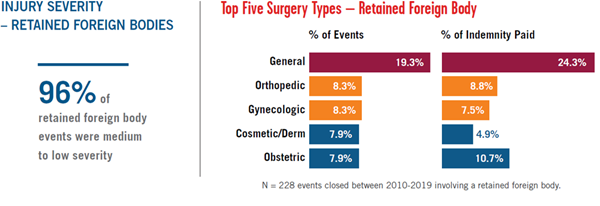
Risk Recommendations for Retained Foreign Bodies
- Identify procedures and patients with a high potential for retained foreign bodies (FBs), for example: obese patients undergoing extensive abdominal surgery.
- Define the responsibilities of the individual tasked with tracking FBs to include tracking of sponges, towels, sharps, and equipment used during procedures. Assign these tasks to a specific individual on the team.
- Limit distractions in the operating room by prohibiting cellphones, music, visitors, and limiting conversations to those required during the procedure.
- Implement assistive technology to identify soft products such as sponges, packing, and towels.
Hospital-Acquired Infections
The number of hospital-acquired infection events, including methicillin-resistant staphylococcus aureus (MRSA), Clostridium difficile (c.diff), sepsis, etc., is low but rising slowly. Diagnosis-related allegations account for 80% of indemnity paid for hospital-acquired infections.
While only 3% of events resulted in high-severity injury outcomes, the payouts on those cases were significant:
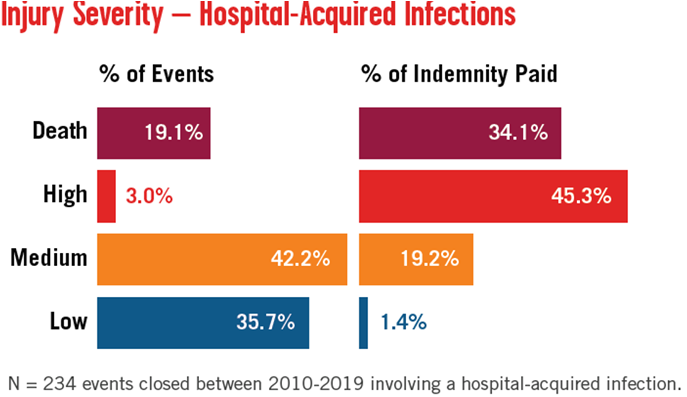
For more information about communication, retained foreign bodies, and hospital-acquired infection risks, please refer to pages 25–28 within A Call for Action: Insights From a Decade of Malpractice Claims.
Copyrighted. No legal or medical advice intended. This post includes general risk management guidelines. Such materials are for informational purposes only and may not reflect the most current legal or medical developments. These informational materials are not intended, and must not be taken, as legal or medical advice on any particular set of facts or circumstances.




